Initial Method
In most who do not have a difficult airway (as assessed on airway exam), direct larygnoscopy will be used when the patient required sedation. Other options for providing operative ventilation include:
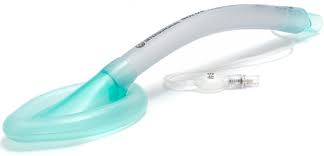
1. Laryngeal Mask Airway (LMA): Useful for short cases. Contraindications include aspiration risk (as positive pressure can still be transferred to the lower esophageal sphincter), supraglottic airway abnormalities, and complete upper airway obstruction.
2. Awake Fiberoptic Intubation: Indicated in patients who may be difficult to ventilate, have a difficult airway (i.e. difficult to intubate), aspiration risk with a contraindication to succinylcholine (i.e. cannot receive rapid sequence intubation), inability to access pre-cricoid or pre-tracheal region (i.e. difficulty creating an invasive airway), or patients with unstable C-spines (e.g. due to RA or trauma).
Contraindicated in difficult airway with impending obstruction, upper airway infection, uncooperative patient.
Difficult intubation
- After a failed attempt at intubation, begin ventilating the patient.
- Change provider, blade, or patient position and try again. If you succeed, be sure to give the patient steroids to reduce inflammation/reduce post-op soreness.
- If direct laryngoscopy fails again, consider alternatives such as an LMA, a video laryngoscope, or a fiberoptic intubation.
If the patient cannot be ventilated: This is an airway emergency. Do the following:
- Call for Help.
- Change patient's position of try placing an LMA to rescue the airway.
- If this isn't successful, you have two options: An emergency airway is required, which can be invasive (i.e. a tracheostomy or a cricothyroidectomy) or Non-Invasive (Rigid Bronchoscopy, Transtracheal Jet Ventilation).